The pediatric to adult transition of care letter is a vital document ensuring medical continuity for young adults moving to adult healthcare systems. It summarizes clinical history, active treatments, and self-management goals to prevent gaps in treatment. Proper documentation empowers patients and informs new providers during this critical life stage. To simplify your process, below are some ready to use template.

Letter Samples List
- Pediatric Transition Introduction Letter for Adolescent Patients
- Parent and Guardian Transition of Care Notification Letter
- Adult Primary Care Provider Medical Referral Letter
- Patient Medical Records Transfer Authorization Letter
- Comprehensive Clinical Care Summary Transition Letter
- Welcome to Adult Care Clinic Introduction Letter
- Chronic Condition Management Transition Letter
- Prescription and Medication Transfer Verification Letter
- Transition Readiness Assessment Acknowledgment Letter
- Medical Insurance and Billing Transition Information Letter
- Emergency Medical Action Plan Transfer Letter
- Pediatric Clinic Farewell and Final Discharge Letter
Pediatric Transition Introduction Letter for Adolescent Patients
A Pediatric Transition Introduction Letter is a vital tool for adolescent patients moving toward adult healthcare. This document summarizes their medical history, current medications, and ongoing treatment needs. It ensures a seamless transfer of care by providing adult providers with essential clinical context. By fostering healthcare autonomy, the letter empowers young adults to manage their own wellness. It acts as a bridge, reducing risks of care gaps and ensuring that care continuity remains a priority during this significant life milestone.
Parent and Guardian Transition of Care Notification Letter
The Parent and Guardian Transition of Care Notification Letter is a formal document used to inform families when a minor transitions from pediatric to adult healthcare services. This communication ensures a seamless continuity of care by detailing the transfer of medical records, identifying new specialists, and outlining upcoming legal changes regarding healthcare decision-making. Providing this notice early helps families prepare for the shift in responsibility, preventing gaps in treatment and ensuring that the young patient's medical history remains accessible during the clinical handover process.
Adult Primary Care Provider Medical Referral Letter
An Adult Primary Care Provider Medical Referral Letter is an essential clinical document facilitating the transition of patient care to a specialist. It must clearly outline the reason for referral, relevant medical history, and current medications to ensure continuity. This professional communication optimizes diagnostic accuracy and streamlines the treatment plan. Providing precise clinical data helps specialists prioritize urgent cases, ultimately improving patient outcomes through coordinated healthcare delivery. Accurate documentation remains the cornerstone of effective interdisciplinary collaboration in modern medicine.
Patient Medical Records Transfer Authorization Letter
A Patient Medical Records Transfer Authorization Letter is a formal legal document required to move private health information between providers. It must explicitly state the patient's identity, the specific records to be released, and the expiration date of the consent. To comply with HIPAA regulations, the letter must include a clear purpose for the transfer and the recipient's contact details. This authorization ensures data privacy while maintaining continuity of care, allowing new specialists to access your clinical history, test results, and prior treatments securely and legally.
Comprehensive Clinical Care Summary Transition Letter
A Comprehensive Clinical Care Summary Transition Letter is a vital document ensuring seamless continuity of care during patient handoffs. It synthesizes complex medical histories, current medications, and pending diagnostic plans into a concise format. This letter bridges the communication gap between pediatric and adult healthcare or between different specialists. By prioritizing patient safety and clear data transfer, it reduces medical errors and ensures the receiving clinician understands the patient's full clinical picture. Accurate summaries are essential for effective clinical care transitions and long-term health management.
Welcome to Adult Care Clinic Introduction Letter
Our Welcome to Adult Care Clinic Introduction Letter serves as a vital foundation for your healthcare journey. This document outlines our comprehensive services, professional medical team, and patient-centered policies to ensure a seamless experience. It provides essential instructions on scheduling appointments, accessing medical records, and understanding insurance procedures. By reviewing this introduction, you gain clarity on how we prioritize your well-being and preventive care. We are committed to fostering a trusted partnership with you, delivering high-quality clinical excellence tailored to your unique adult health needs from the very first visit.
Chronic Condition Management Transition Letter
A Chronic Condition Management Transition Letter is a critical document ensuring continuity of care when a patient moves between healthcare providers. It summarizes medical history, current medications, and ongoing treatment plans to prevent gaps in therapy. This clinical handover facilitates a seamless exchange of information, reducing risks of complications or medication errors. It serves as a roadmap for the receiving physician to maintain the patient's health stability. Clear communication through this letter is essential for effective long-term health outcomes and patient safety during organizational or life changes.
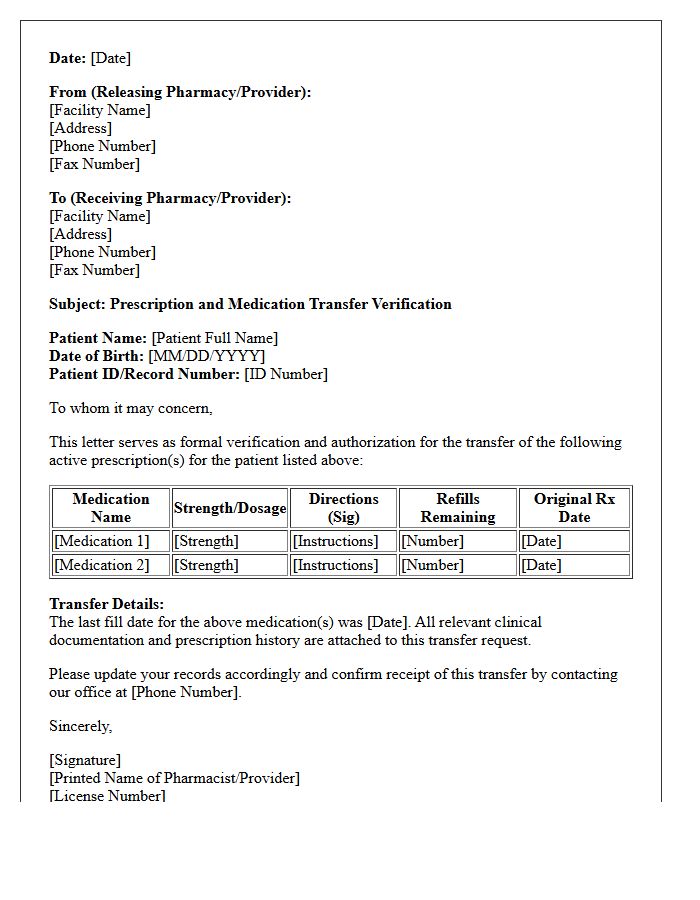
Prescription and Medication Transfer Verification Letter
A Medication Transfer Verification Letter is a formal document used to ensure the safe transition of prescriptions between healthcare providers or pharmacies. It confirms the authenticity of active orders, dosage histories, and clinical necessity to prevent treatment interruptions. This record acts as a legal safeguard for patients moving internationally or switching clinics. It must include the physician's credentials, the patient's diagnosis, and precise pharmaceutical details to verify that continuity of care is maintained according to regulatory standards.
Transition Readiness Assessment Acknowledgment Letter
A Transition Readiness Assessment Acknowledgment Letter is a formal document verifying that a service member has completed the mandatory Pre-Separation Counseling. It serves as official proof that an individual understands their post-military benefits, obligations, and transition requirements. This letter is a critical component of the TAP process, ensuring that personnel are prepared for civilian life. Command signatures on this document confirm that the assessment was conducted according to Department of Defense standards, allowing for a seamless discharge and successful reintegration into the workforce or education sectors.
Medical Insurance and Billing Transition Information Letter
A Medical Insurance and Billing Transition Information Letter is a formal notification sent to patients regarding changes in healthcare coverage or payment systems. It highlights continuity of care by detailing new provider networks, updated billing procedures, and potential adjustments in out-of-pocket costs. Patients must review this document to ensure seamless transitions between insurance plans without service interruptions. Key details often include effective dates and instructions for updating patient records to prevent claim denials. Understanding these updates is essential for maintaining accurate financial records and accessing necessary medical treatments during administrative shifts.
Emergency Medical Action Plan Transfer Letter
An Emergency Medical Action Plan Transfer Letter is a vital document ensuring the continuity of care during patient transitions between facilities. It outlines a patient's current status, critical diagnoses, and immediate treatment protocols. By providing clear clinical instructions to the receiving medical team, it minimizes risks and prevents preventable medical errors. This formal communication serves as a roadmap for healthcare providers, ensuring that life-saving interventions are maintained without delay during high-stakes transfers. Prioritizing accurate data in this letter is essential for effective patient safety and successful emergency outcomes.
Pediatric Clinic Farewell and Final Discharge Letter
A pediatric clinic farewell and final discharge letter marks the transition to adult healthcare. This formal document serves as a medical summary, detailing the patient's history, immunization records, and ongoing treatment plans. It ensures continuity of care by providing the new provider with essential clinical data. Parents should confirm all specialist referrals are included and request a complete copy for their personal archives. This transition typically occurs between ages 18 and 21, ensuring the young adult moves safely into the internal medicine system with a clear health roadmap.
What is a pediatric to adult transition of care letter?
A pediatric to adult transition of care letter is a formal document prepared by a pediatrician that summarizes a young adult's medical history, current diagnoses, medications, and treatment plans to ensure a seamless transfer to an adult healthcare provider.
When should a transition of care letter be prepared?
The transition process typically begins between ages 14 and 16, but the formal transition letter is usually finalized and sent to the new adult primary care physician when the patient is between 18 and 21 years old.
What key information is included in a medical transition summary?
A comprehensive transition letter includes a summary of chronic conditions, surgical history, immunization records, current medication dosages, known allergies, and the contact information for any active specialists.
Why is a formal transition letter necessary for young adults with special healthcare needs?
For patients with complex or chronic conditions, a formal letter prevents gaps in care, ensures the new provider understands the nuances of previous treatments, and helps maintain insurance authorizations for necessary therapies or equipment.
How can I request a transition of care letter from my pediatrician?
You can request a transition letter by scheduling a "transition visit" with your pediatrician. During this appointment, you should confirm that all records are updated and provide the name and fax number of the adult practitioner who will be taking over your care.














Comments